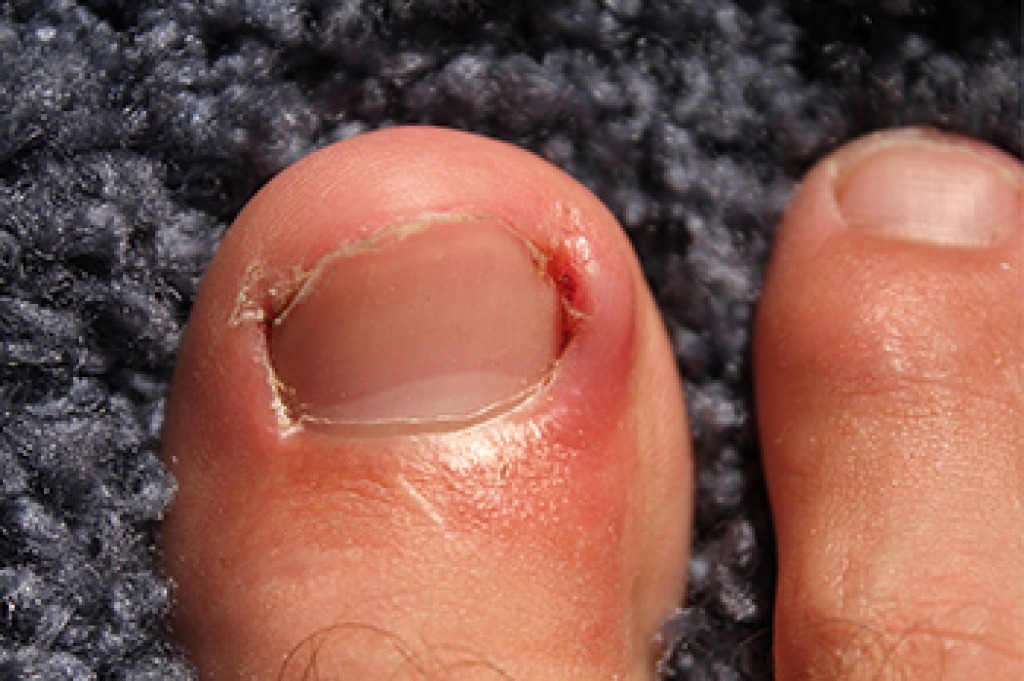
Diabetic neuropathy is a type of nerve damage linked to diabetes that commonly affects the feet and lower legs. High blood sugar can damage nerves, causing numbness, tingling, burning pain, and sharp shooting sensations in the feet. Some people lose the ability to feel heat, cold, or injuries, which increases the risk of cuts, blisters, and foot ulcers going unnoticed. Changes in sensation can also affect balance and stability when walking, increasing the risk of falls. Because feeling in the feet becomes reduced, small wounds can develop into serious infections. A podiatrist can examine the feet, check for nerve damage, monitor circulation, and provide treatment to help prevent further complications. Early care is important for protecting foot health and lowering the risk of severe infections or long-term tissue damage. If you have symptoms of diabetic neuropathy, it is suggested that you schedule an appointment with a podiatrist for expert guidance in managing this condition.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with Jeffrey Radack, DPM from Texas Regional Foot & Ankle Clinics. Our doctor will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
- Numbness
- Sensation loss
- Prickling and tingling sensations
- Throbbing, freezing, burning pains
- Muscle weakness
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact our office located in McKinney and Coppell, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.